Ayushman Bharat: India’s Flagship Healthcare Reform and Its Expanding Impact
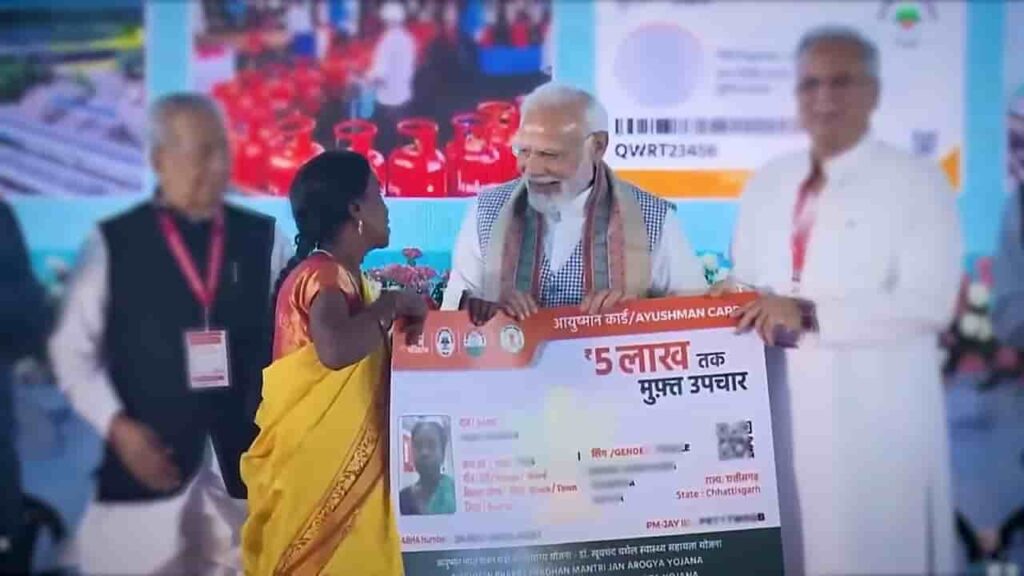
Ayushman Bharat has been one of the most ambitious and transformative public healthcare initiatives undertaken in India, aimed at addressing long-standing gaps in accessibility, affordability, and quality of medical services. Launched in 2018 by the Government of India, the programme was conceptualised as a comprehensive reform to strengthen the country’s healthcare system at multiple levels—from preventive care at the grassroots to financial protection during critical illnesses.Over time, Ayushman Bharat has not only expanded its coverage but also redefined how healthcare is accessed by economically vulnerable populations, making it a central pillar of India’s public health policy.Background: Why Ayushman Bharat Was IntroducedBefore the introduction of Ayushman Bharat, a significant portion of India’s population faced serious challenges in accessing healthcare. High out-of-pocket expenditure, limited insurance coverage, and inadequate primary healthcare infrastructure meant that medical emergencies often pushed families into financial distress.India’s healthcare system had long been characterised by:Heavy reliance on private healthcare servicesHigh treatment costs without financial protectionLimited access to quality care in rural areasFragmented public health infrastructureAyushman Bharat was introduced to address these structural issues by creating a system that combines preventive, promotive, and curative healthcare under a single framework.The Two-Pillar Structure of Ayushman BharatThe programme was designed with a dual approach, ensuring that both basic healthcare needs and advanced medical treatments are covered.1. Health and Wellness Centres (HWCs)The first component focused on strengthening primary healthcare by transforming existing sub-centres and primary health centres into Health and Wellness Centres.These centres were developed to provide comprehensive primary healthcare services, moving beyond limited treatment facilities to include:Maternal and child health servicesImmunisation programmesScreening and management of non-communicable diseases such as diabetes and hypertensionMental health servicesFree essential medicines and diagnosticsPreventive healthcare and awareness programmesThe emphasis on preventive care marked a shift in approach—from treating illness to promoting overall health and early diagnosis.2. Pradhan Mantri Jan Arogya Yojana (PM-JAY)The second and more widely recognised component is Pradhan Mantri Jan Arogya Yojana (PM-JAY), which provides financial protection for hospitalisation.PM-JAY has been designed as a government-funded health insurance scheme, offering:Coverage of up to ₹5 lakh per family per yearAccess to both public and empanelled private hospitalsCashless and paperless treatment at the point of serviceCoverage for a wide range of medical procedures, including surgeries and specialised treatmentsThe scheme primarily targets economically weaker sections, identified through socio-economic data, ensuring that those most in need receive support.Scale and Reach of the ProgrammeAyushman Bharat has been recognised as one of the largest healthcare schemes in the world, covering over 50 crore beneficiaries across India.The scale of the programme is reflected in:Thousands of empanelled hospitals across statesExpansion of Health and Wellness Centres in both rural and urban areasLarge number of hospital admissions under PM-JAYIncreasing awareness and enrolment among eligible populationsThe wide reach of the scheme has played a critical role in bridging healthcare gaps, particularly in underserved regions.Key Features and Operational FrameworkThe effectiveness of Ayushman Bharat lies in its structured implementation and use of technology.Some of its notable features include:Cashless Treatment: Beneficiaries can avail treatment without making upfront paymentsPortability: Services can be accessed across India, irrespective of the beneficiary’s home stateDigital Integration: Use of digital health cards, online verification, and real-time claim processingFraud Control Mechanisms: Systems to monitor and prevent misuse of fundsThese features have made the scheme more accessible, transparent, and efficient.Impact on Healthcare AccessibilitySince its implementation, Ayushman Bharat has had a significant impact on healthcare access in India.It has contributed to:Increased hospital admissions among low-income groupsReduced financial burden during medical emergenciesGreater utilisation of private healthcare facilitiesImproved access to specialised treatments that were previously unaffordableFor many beneficiaries, the scheme has acted as a critical safety net, enabling them to seek timely medical care without fear of financial hardship.Economic and Social ImplicationsBeyond healthcare, Ayushman Bharat has had broader socio-economic implications.By reducing out-of-pocket expenditure, the scheme has helped prevent families from falling into poverty due to medical expenses. It has also:Encouraged investment in healthcare infrastructureCreated employment opportunities in the health sectorPromoted public-private partnerships in healthcare deliveryAdditionally, improved health outcomes contribute to increased productivity and overall economic growth.Challenges in ImplementationDespite its achievements, the programme has faced certain challenges that have influenced its effectiveness.These include:Uneven implementation across statesLimited infrastructure in remote and rural areasAwareness gaps among eligible beneficiariesOccasional delays in claim settlementsConcerns regarding quality of care in some empanelled hospitalsAddressing these challenges has remained crucial for ensuring that the benefits of the scheme reach all intended recipients.Integration with India’s Digital Health EcosystemAyushman Bharat has also played a role in advancing India’s digital health initiatives. The integration of technology has enabled better tracking of patient data, streamlined service delivery, and improved transparency.The move toward digital health records and interconnected systems is expected to further strengthen the healthcare ecosystem in the long run.A Step Toward Universal Health CoverageAyushman Bharat has been a key step in India’s journey toward achieving universal health coverage. By combining primary healthcare reforms with financial protection, the scheme has addressed multiple dimensions of healthcare delivery.It reflects a shift in policy focus—from limited, fragmented healthcare services to a more inclusive and structured system that prioritises accessibility and affordability.Ayushman Bharat has, over the years, reshaped the way healthcare is accessed and delivered in India. By reducing financial barriers, expanding infrastructure, and promoting preventive care, it has moved the country closer to a more equitable healthcare system—one where access to treatment is determined not by income, but by need.
Russia Develops Experimental Cancer Vaccine, Early Trials Show Promise

Russia has announced the development of an experimental cancer vaccine, marking a significant step in its ongoing efforts to advance personalised cancer treatment through immunotherapy. The vaccine, which is still in the research and clinical trial stage, has been developed by scientific institutions operating under Russia’s state-run medical research framework and is being positioned as a therapeutic vaccine, not a preventive one. According to Russian health authorities, the vaccine is designed to stimulate the patient’s immune system to recognise and attack cancer cells, rather than prevent the onset of cancer. This places it within the rapidly growing global field of cancer immunotherapy, where treatments are tailored to the biological profile of an individual’s tumour. What Makes the Vaccine Different Unlike conventional vaccines used against infectious diseases, Russia’s cancer vaccine is personalised. It is developed using messenger RNA (mRNA) technology, a platform that delivers genetic instructions to the body’s cells, enabling the immune system to identify tumour-specific antigens and mount a targeted response against cancer cells. Russian researchers have stated that the vaccine is created after genetic sequencing of a patient’s tumour, allowing the formulation to be customised for each individual. This approach aims to improve treatment precision while reducing damage to healthy cells — a longstanding challenge in traditional cancer therapies such as chemotherapy and radiation. The project is being led by institutions under the Federal Medical Biological Agency (FMBA), with collaboration from leading molecular biology and oncology research centres in Russia. Stage of Development and Trials Russian officials have clarified that the vaccine has completed pre-clinical testing and has entered early-phase human trials, primarily focused on assessing safety and immune response rather than long-term efficacy or cure rates. Preliminary observations from these early trials suggest that the vaccine has triggered immune activation against cancer cells, with researchers reporting an absence of severe adverse effects among participants. However, experts stress that Phase I trials are not designed to establish effectiveness, and broader conclusions can only be drawn after larger Phase II and Phase III trials. As of now, comprehensive peer-reviewed clinical data has not been published in international medical journals, and the vaccine has not received regulatory approval for widespread clinical use either within Russia or internationally. Not a “Cancer Cure” Medical experts and health authorities have cautioned against describing the development as a cure for cancer. Cancer is not a single disease but a complex group of conditions, and therapeutic vaccines are generally intended to slow disease progression, prevent recurrence, or improve survival outcomes, often in combination with other treatments. Independent analysts have pointed out that while early results are encouraging, claims circulating on social media suggesting “100 per cent effectiveness” are scientifically inaccurate and misleading. Regulatory approval will depend on long-term trial outcomes, reproducibility of results and transparent data validation. International Interest and Future Plans Despite its early stage, the announcement has drawn international attention, with some countries reportedly expressing interest in observing or participating in further clinical evaluation once larger trials are initiated. Russian health authorities have indicated that, subject to successful trial outcomes and regulatory clearance, limited clinical use could be expanded in the coming years, particularly for cancers where existing treatments show limited effectiveness. Why This Development Matters Globally, cancer remains one of the leading causes of death, and the pursuit of personalised, less toxic treatments is a major priority for medical research. Therapeutic cancer vaccines, especially those using mRNA technology, are seen as a promising frontier because they aim to harness the body’s own immune defences rather than relying solely on invasive treatments. Russia’s progress reflects a broader global shift towards precision medicine, where treatments are increasingly tailored to individual patients rather than applied uniformly. The Road Ahead For now, Russia’s cancer vaccine remains an experimental medical innovation, not a commercially available treatment. Scientists and clinicians agree that extensive clinical trials, peer-reviewed data and international regulatory scrutinywill be critical before the vaccine can be considered a reliable addition to cancer care. While the early findings offer cautious optimism, experts emphasise that rigorous science, not headlines, will determine whether the vaccine ultimately changes cancer treatment outcomes.
Clascoterone Breakthrough Boosts Hair Growth by Up to 539%, Offering New Hope Against Baldness
After decades of limited progress in male-pattern baldness treatment, new clinical data released this month have generated a wave of optimism in the dermatology and biotech communities.Clascoterone 5% topical solution, developed by Irish-based Cosmo Pharmaceuticals, has shown remarkably strong results in late-stage clinical trials, including up to a 539% relative improvement in hair count compared with placebo in one study.The results, drawn from two identically designed Phase III trials named SCALP-1 and SCALP-2, represent the largest late-stage clinical program ever conducted for a topical hair-loss treatment. Together, these studies enrolled 1,465 men across the United States and Europe with androgenetic alopecia, the most common form of hair loss worldwide.In SCALP-1, participants using clascoterone showed a 5.39-fold (539%) relative increase in target-area hair count compared with those receiving a placebo vehicle. The second trial demonstrated a 1.68-fold (168%) improvement over placebo. Both results met strict statistical significance thresholds. Why This Matters? Male-pattern baldness, or androgenetic alopecia (AGA), affects a huge portion of the global population, with some estimates suggesting over 1 billion men are impacted. Current treatment options include oral medication like finasteride and topical minoxidil.Clascoterone works differently. Instead of interfering with the hormone system-wide, it blocks dihydrotestosterone (DHT) locally at the hair follicle, the hormone widely understood to shrink hair roots and trigger thinning in genetically predisposed individuals. By acting directly on the scalp with minimal systemic absorption, clascoterone aims to reduce common side effect concerns associated with oral treatments.Early patient-reported outcomes also supported the objective findings, with many users noting visible regrowth and satisfaction, an encouraging sign that the statistical benefits translated into meaningful change for subjects in the trials. Safety and the Path Ahead Safety data from the trials are promising. Incidences of treatment-emergent adverse events were comparable to placebo, indicating a favorable tolerability profile.Cosmo Pharmaceuticals is now completing an additional 12-month safety and durability study, expected by spring 2026, after which it plans parallel regulatory submissions to U.S. and European authorities.If approved, clascoterone could become the first novel topical hair-loss mechanism in over 30 years, a milestone many clinicians have long awaited.While not a guaranteed “cure,” these results may reshape the therapeutic landscape for millions struggling with hair loss and could launch a new era of effective, topical solutions.


